Jitendra Chouksey, founder of Fittr and a man who has built a following by asking uncomfortable questions, recently walked into a minefield and detonated it himself. His LinkedIn post, provocatively titled “The Cervical Cancer Vaccine Scam!”, set off a firestorm.
Doctors, pathologists, and oncologists pushed back hard and fast. Social media split down the middle. And somewhere in the noise, a genuinely important conversation got buried under an irresponsible headline. Let’s untangle this, fairly, and without taking sides just for the sake of taking sides.
What Chouksey Got Wrong
Let’s start here, because this matters. Calling cervical cancer vaccination a “scam” is not a critique. It is a provocation. And provocations, however good the intention behind them, do not save lives, they cost them.
Cervical cancer is one of the most preventable cancers in the world. The HPV vaccine, which targets the strains of the Human Papillomavirus strains 16 and 18 – responsible for about 70% of cervical cancers, has decades of clinical evidence behind it. Countries that have implemented high‑coverage HPV vaccination programmes have seen dramatic declines in HPV‑16/18 infection, precancerous lesions, and, more recently, in invasive cervical cancer incidence.
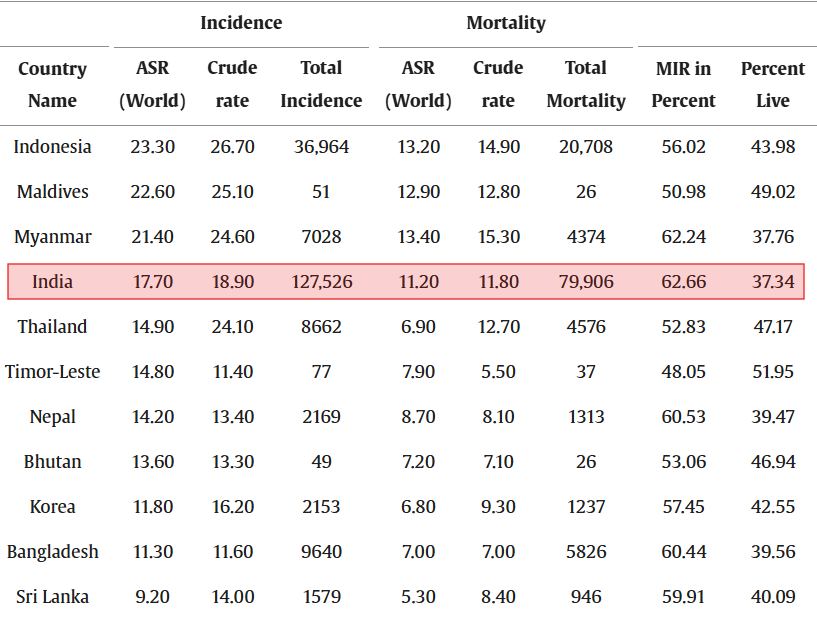
In India, official data from the Indian Council of Medical Research–National Cancer Registry Programme (ICMR–NCRP) estimates 35,691 cervical cancer deaths in 2023, up from 34,806 in 2022. By contrast, global estimates from GLOBOCAN 2022 place the toll at about 79,906 cervical cancer deaths per year, reflecting a more aggressive attempt to correct for under‑counting in countries with weak death‑certification systems.
These figures are model‑based and imperfect, but they are not arbitrary scare‑mongering; they are the best available estimates, built from India’s partial cancer registries on one hand and global statistical modelling on the other.
Women are being diagnosed. Lifetimes are being derailed. In many instances, particularly in tier‑2 and tier‑3 cities, women reach hospitals only when the disease is advanced, because screening (like VIA) often misses early lesions and awareness remains patchy.
When someone with a large platform tells their audience that the vaccine is a scam and proudly declares they will not vaccinate their daughter, they are not being brave. They are being reckless. For every person who critically evaluates that claim, there are many who will remember the word “scam” the next time a doctor recommends the vaccine for their child.
The medical community’s outrage was not fragile defensiveness. It was the sound of people who see the consequences of misinformation up close, every single day.
What Chouksey Got Right – Even If He Got There the Wrong Way
Here is where we need to be honest and uncomfortable. Chouksey went to the ICMR website and government data portals, the official, go‑to sources that policymakers and regulators rely on and pulled up cervical cancer death data.
What he found was thin. Patchy numbers from earlier years, estimated figures of a few dozen deaths in certain categories, no clear trend, and almost no longitudinal, user‑friendly tracking that builds a compelling, evidence‑based narrative for a national vaccination push.
Now, if one were to reconstruct the prevailing medical‑community mindset, it might sound like this: “Even if the data systems are imperfect, we know the disease is real and the vaccine works. Poor data should not become a pretext to reject sound science.” That reasoning is medically justifiable but institutionally dangerous. Why?
Because ICMR–NCRP and government health portals are not just websites. They are the single most authoritative reference point for health policy in this country. When a regulator, a policymaker, a journalist, or a researcher wants to make a data‑backed argument about cervical cancer, that is where they go. That data is the foundation on which decisions are made, budgets are allocated, and public health campaigns are built.
If that foundation looks dusty, if the dashboards are hard to read, timelines are unclear, and international readers find only archived PDFs instead of intuitive visualisations, it is not a minor inconvenience. It is a systemic failure.
And dismissing the gap with “data isn’t always updated, that’s just how it is” sets a deeply troubling precedent. It essentially says: “Trust the institution, not the evidence.” That is precisely the kind of response that breeds the Choukseys of the world.
This Is Not a Capability Problem. It’s a Priority Problem.
The government can do this, we’ve seen it before. India’s handling of COVID‑19 data, for all its early chaos, eventually became a case study in mobilisation.
The vaccination dashboard, real‑time tracking, district‑level granularity, all of it was built from scratch, under pressure, with no playbook. The government showed, in the most adverse conditions imaginable, that it can collect, process, and communicate health data at scale.
So the question is not “Can we maintain updated, reliable cervical cancer surveillance data?” The question is: “Have we decided that it matters enough?” The answer, evidently, is not yet.
Where the Science Stands and Where the Headline Misleads
Chouksey’s post correctly notes that no phase‑3 randomized controlled trial (RCT) has used invasive cervical cancer as the primary endpoint. Instead, trials measure CIN2 and CIN3 lesions, cervical intraepithelial neoplasia stages that are early, abnormal changes in cervical cells.
He calls these “unreliable markers”; in reality, CIN2/CIN3 are widely accepted early warning signs of cancer risk, even though not all lesions progress to cancer. Many CIN2 cases regress on their own; only a subset progress to CIN3; and not all CIN3 lesions become cancer.
But the vaccine’s job is not to treat existing lesions. It is to prevent HPV infection in the first place, typically given to girls aged 9-14, ideally before sexual activity. Thanks to that upstream prevention, large trials like FUTURE II (over 12,000 women) found that Gardasil reduced high‑grade CIN3+ lesions by about 98% among HPV‑naïve women. The PATRICIA trial (over 18,000 women) showed Cervarix cutting CIN3+ by about 93%. These are not “tricks” of statistics; they are rigorous, long‑term clinical signals.
Real‑world data followed. A landmark 2020 Swedish cohort study of about 1.7 million women, later extended with an 18‑year follow‑up and published in The BMJ, found that girls vaccinated against HPV before age 17 had about 80–90% fewer invasive cervical cancers compared with unvaccinated peers. This is observational, not a randomised trial, but it is one of the cleanest real‑world validations of HPV vaccination anywhere.
The ‘0.045% Help vs 0.3% Harm’ Claim And Why It’s Misleading
Chouksey’s central math claim is that the absolute risk reduction (ARR) of cervical cancer from HPV vaccines is about 0.045%, drawn from the Swedish study, while the absolute “harm” from the FUTURE trials is about 0.3% (serious adverse events like hospitalisations or disabilities). On paper, that looks like harm outweighs benefit, especially when you’re talking about healthy girls.
But this framing is highly selective and misleading.
- The Swedish study’s 0.045% ARR is a rough, simplified translation of a very small absolute risk over one year, pulled out of a long‑term observational design. Cervical cancer risk builds over decades, and the 88% relative reduction is far more meaningful than the tiny yearly percentage.
- The 0.3% ‘harm’ figure comes from a 2017 critical review by Martínez‑Lavín, who reported 3.3% serious adverse events in the 9‑valent HPV vaccine arm versus 2.6% in the 4‑valent HPV‑placebo arm, but acknowledged that many events were not clearly vaccine‑related.
The FUTURE II trial itself reported that serious adverse events occurred in 0.2% of vaccinated women versus 0.1% in the placebo group, with no deaths attributed to the vaccine. The WHO’s global safety review of more than 500 million Gardasil doses, spanning years and continents, finds severe allergic reactions in about 1.7 per million doses, and no proven causal link to chronic or ongoing illnesses.
So medically, the picture is clear: the HPV vaccine prevents thousands of cervical cancer cases across a population at extremely low risk of serious harm.
Why Doubts Linger in India
The Indian rollout makes the math abstract for many families. Launched on 28 February 2026 by Prime Minister Narendra Modi, the nationwide free HPV vaccination programme targets about 1.2 crore girls aged 14, using Gardasil‑4 procured via the Gavi alliance.
Public hesitation persists for several reasons:
- Past controversies, such as the 2010 HPV trial in Andhra Pradesh, where seven deaths occurred post‑vaccination, later deemed unrelated to the vaccine by investigators, have damaged trust.
- Opaque communication and fears of pharmaceutical influence fuel suspicion.
- Misleading framing is common: benefits are often presented in relative terms (e.g., 90% reduction in CIN3), which sounds huge, while harms are described in absolute terms, which can feel scarier. This is a known pattern in medical reporting, but it can mislead people who don’t read the fine print.
Doctors also know that screening methods like VIA (visual inspection with acetic acid) have limited sensitivity: roughly 60–70% of cervical cancer cases in India present at late stages, despite some screening efforts. That’s why vaccination is considered upstream prevention, not a replacement for screening, but a complementary tool.
Cervical Cancer Is Not a Scam. The System Is Partly to Blame.
The internet is now divided: doctors on one side, Fittr fans on the other, and a largely confused public in the middle wondering who to trust. That division is not Chouksey’s fault alone. It is the fault of a system that allowed a credibility vacuum to exist in the first place.
When official data are sparse, hard to access, or poorly visualised, influencers fill the gap. When institutions don’t communicate proactively and clearly, provocateurs do. The antidote to bad‑faith health communication is not just fact‑checking and outrage, it is radical, accessible, rigorously updated public‑health data.
Cervical cancer is not a scam. The HPV vaccine is not a conspiracy. Women are being diagnosed, treated, and, in too many cases, lost to a disease that we have proven tools to prevent. But Jitendra Chouksey accidentally pointed a flashlight at a real problem: our national health data infrastructure for non‑pandemic diseases is underfunded, under‑prioritised, and under‑communicated.
That is a conversation worth having. Just not under a headline that calls it a “cervical cancer vaccine scam.”
Bridging the Data Gap with Concrete Fixes
India’s cervical‑cancer numbers look wildly different under GLOBOCAN and ICMR–NCRP because each system corrects for under‑reporting in its own way, global models inflate, while national registries stay conservative. Turning this crisis into opportunity means building a more transparent, real‑time health‑data infrastructure grounded in actual evidence.
- Build a unified, real‑time national health‑data platform that integrates cancer‑registry data, death‑certification records, and hospital‑based surveillance to close the gap between GLOBOCAN‑style global estimates and ICMR‑NCRP‑style national projections.
- Expand population‑based cancer registries into rural and tier‑2 districts, using lessons from the Million Death Study and ICMR‑linked burden‑of‑cancer papers that show large under‑counting in non‑urban areas, to generate more accurate, sub‑national estimates.
- Mandate standardized cause‑of‑death coding and digital reporting across all states, following WHO‑recommended verbal‑autopsy and ICD‑based protocols, to reduce the “missed‑in‑reporting” fraction that drives upward global corrections like GLOBOCAN’s inflated cervical‑cancer numbers.
- Launch public‑health “data‑transparency drives” where ministries regularly publish and explain discrepancies between global models and national estimates, using examples from cervical‑cancer burden studies, so that platforms like Fittr’s need not second‑guess the credibility of official statistics.
Editor’s Note: This article is part of The Logical Take, a commentary section of The Logical Indian. The views expressed are based on research, constitutional values, and the author’s analysis of publicly reported events. They are intended to encourage informed, responsible dialogue around health communication and data transparency, and do not seek to target or malign any individual, institution, or community.













