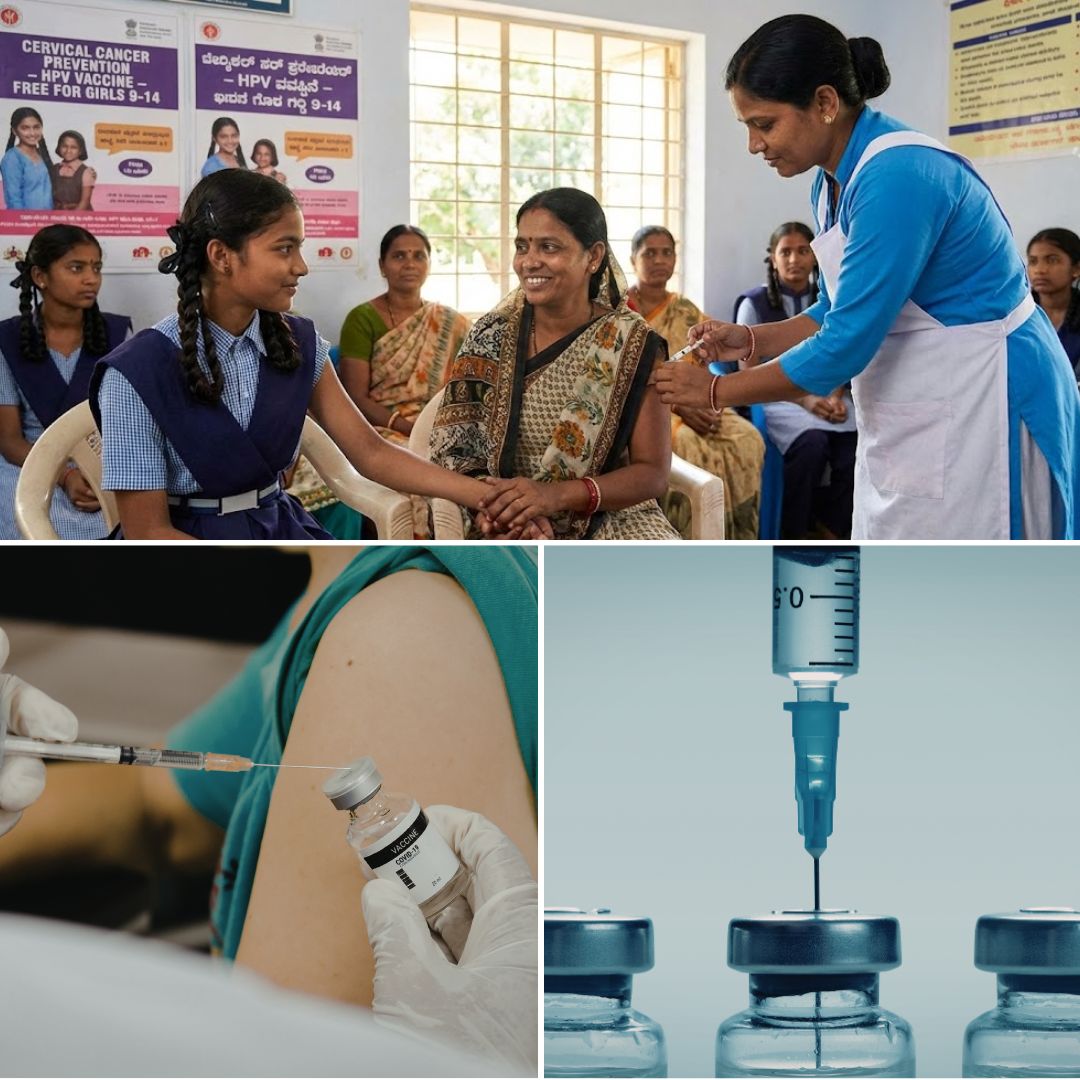
The Union government of India is poised to launch a nationwide Human Papillomavirus (HPV) vaccination programme targeting girls aged 14 years and above, offering the quadrivalent Gardasil vaccine free of cost through designated government health facilities under the Universal Immunisation Programme.
Official sources say the initiative part of the government’s larger “Swastha Nari” preventive health mission will be voluntary, evidence-based, scientifically supported, and designed to significantly reduce India’s cervical cancer burden.
Vaccinating girls before exposure to HPV can prevent most cases of cervical cancer a disease that continues to claim tens of thousands of lives annually in India. The rollout demonstrates a convergence of policy prioritisation, public health preparedness, and expanded vaccine access to achieve long-term cancer prevention.
Nationwide Rollout Details and Government Strategy
According to official sources within the Ministry of Health and Family Welfare, the nationwide HPV vaccination programme will provide the Gardasil quadrivalent vaccine free of cost to eligible girls aged 14 years and above.
The government has underscored that the vaccination exercise will be voluntary and accessible irrespective of socio-economic status, with trained healthcare teams administering doses at Ayushman Arogya Mandirs, Primary Health Centres, Community Health Centres, Sub-District and District Hospitals, and Government Medical Colleges. To ensure safety and confidence among parents, all vaccination sessions will be linked to 24×7 medical facilities capable of managing any rare adverse events following immunisation (AEFI).
Senior officials emphasise that strong global and Indian scientific evidence supports the effectiveness of HPV vaccines and the use of a single-dose schedule for adolescent girls in the recommended age group before potential exposure to the virus.
This approach mirrors international research and World Health Organization guidance that such vaccinations can provide robust and durable immune protection, making it optimally effective in adolescents prior to HPV infection. It also aligns with emerging global practices with over 160 countries incorporating HPV vaccination into national immunisation schedules, and many adopting single-dose strategies to improve coverage and affordability.
Cervical Cancer Burden Demands Urgent Action
Cervical cancer remains a critical public health concern in India. Government and global health data show that the country accounts for roughly one-third of global cervical cancer cases, with tens of thousands of new diagnoses and deaths each year. India continues to report a heavy disease burden, with nearly 80,000 new cases and more than 42,000 deaths annually despite the fact that persistent infection by high-risk HPV types is nearly always preventable through vaccination and early screening.
The quadrivalent Gardasil vaccine which protects against HPV types 16 and 18, known to cause the majority of cervical cancers, as well as types 6 and 11 has an established safety record supported by decades of global use. Experts and official sources note that HPV vaccines are among the most extensively studied immunisations worldwide, demonstrating high effectiveness in preventing disease caused by covered HPV types. Immunising adolescents before exposure to the virus significantly reduces infection risk and subsequent cancer development later in life.
While the current nationwide plan focuses on girls aged 14 and above, state-level pilot programmes and efforts have been underway in parts of India. For example, earlier initiatives in Tamil Nadu and others have provided valuable implementation experience and increased awareness among communities helping build momentum for a broader national rollout. Furthermore, districts like Bhagalpur have already begun single-dose HPV vaccination drives for schoolgirls, emphasising the importance of early immunisation and proactive community engagement.
Challenges, Context, and Lessons from Other Regions
Although the nationwide launch has widespread support from health authorities and global partners, implementation hurdles remain in terms of awareness, misinformation and logistical challenges. Past experiences in other countries, like Pakistan, show how disinformation can dramatically reduce vaccine uptake, leading to poor campaign outcomes despite medical evidence supporting HPV immunisation. Such challenges highlight the importance of effective communication strategies, community trust-building, and accurate public health information to counter misconceptions about vaccines.
Efforts to scale up HPV vaccination also dovetail with broader healthcare priorities. For many years, Indian health experts emphasised the need to strengthen routine screening and prevention programmes alongside immunisation recognising that vaccination alone, while powerful, must be paired with robust cervical cancer screening strategies to detect precancerous lesions and ensure early treatment for all women. The World Health Organization continues to recommend that HPV vaccination at ages 9-14 be part of a comprehensive approach to cervical cancer prevention when integrated with screening and treatment services.
The Logical Indian’s Perspective
India’s decision to launch a nationwide HPV vaccination programme for adolescent girls marks a significant moment in preventive public health. It reflects a long-overdue shift from reactive disease management to proactive, evidence-based prevention a move that could save countless lives, reduce healthcare costs, and transform the health prospects of future generations.
Offering the vaccine free of cost and making it accessible through government health infrastructure demonstrates equity and social justice in public health policymaking. However, vaccination campaigns succeed only when coupled with trust, awareness and informed choice. Clear communication, community engagement, and culturally sensitive outreach are essential to dispel myths and build confidence among parents and guardians.
Read more: ‘Aniyan, Come Down’: How Kerala Police’s Single Word of Empathy Saved a Life in Kozhikode, Kerala